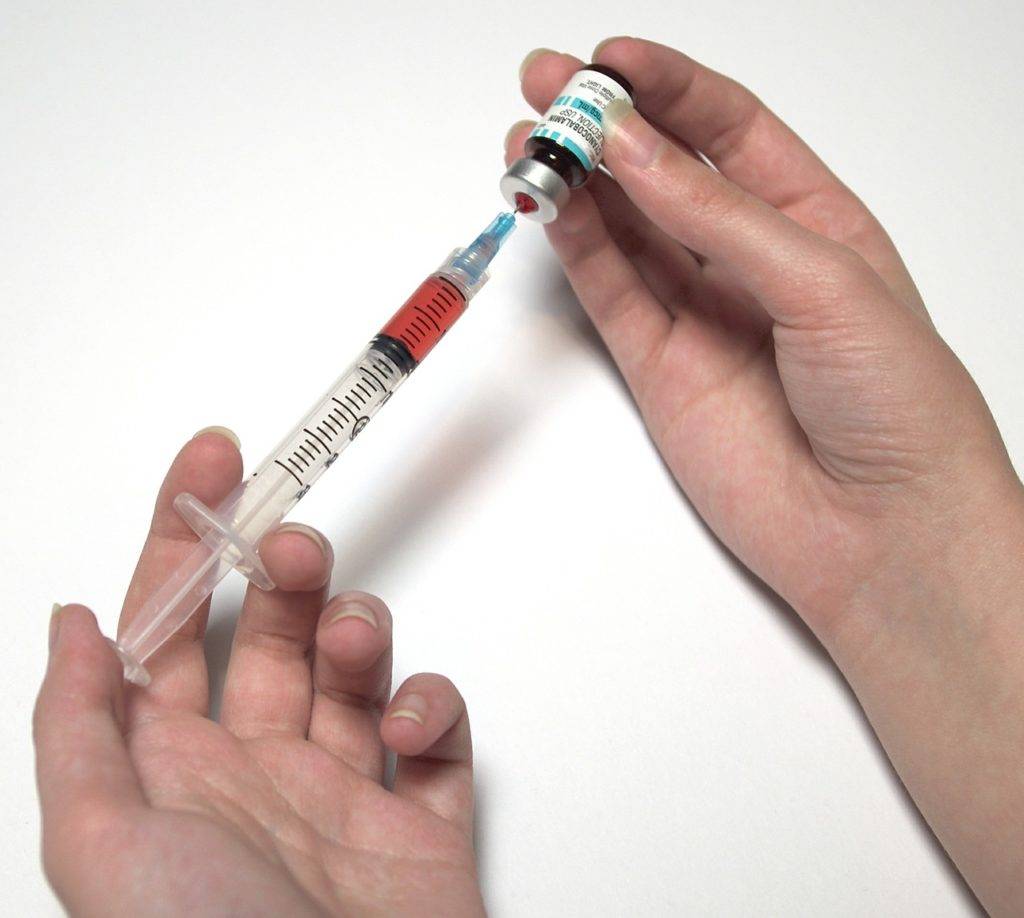
Every parent wants to protect their newborn from harm. When it comes to preventing Hepatitis B (HBV) in babies, the combination of a birth-dose vaccine and, in some cases, Hepatitis B Immune Globulin (HBIG) matters.
This article will explore which infants still need HBIG at birth and why, when, and how you, as a parent or caregiver, can help make sure your baby is safe.
What is HBIG—and Why Do We Care?
Before we talk about who needs it, let’s define the key players:
- The hepatitis B virus (HBV) is a liver-infecting virus that can pass from a person who has it to another. When a baby is exposed to the mother at or around birth, the risk of chronic infection is high.
- The hepatitis B vaccine (birth dose) is given to all infants (in many countries) as the very first dose of the series. It stimulates the baby’s immune system to protect against HBV.
- HBIG is a preparation of antibodies given to a baby right after birth (post-exposure) to give immediate protection while the vaccine takes effect. Think of it as the “shield” while the “training” (vaccine) begins.
- The reason: if a baby is exposed to HBV during birth (since the mother is infected or might be), without this combination, the baby is at very high risk of becoming chronically infected—which can lead to long-term liver damage, cirrhosis, or liver cancer.
Thus, HBIG is not for every baby at birth—but is very important in certain risk situations.
The Big Picture: When Do All Babies Get the Hepatitis B Vaccine, and When Do They Get HBIG?
Here’s a summary:
- All babies: In many countries (including the US), all newborns should receive the birth dose of the hepatitis B vaccine (within 24 hours of birth) regardless of the mother’s HBV status.
- Some babies also get HBIG at birth. These babies are those at higher risk of HBV exposure.
- The key factors: The mother’s infection status (specifically, HBsAg positive = hepatitis B surface antigen positive, meaning she is infected) or unknown; the baby’s birthweight (very low birthweight < 2000 grams); and whether the baby’s vaccine starts on time.
We’ll go into the details below: Which infants still need HBIG at birth in today’s guidelines?
Which Infants Still Need HBIG at Birth?
According to current CDC guidelines and other sources, here’s a breakdown of scenarios based on maternal status and infant characteristics.
 1. Mother known to be HBsAg-positive
1. Mother known to be HBsAg-positive
If the mother’s hepatitis B surface antigen (HBsAg) test is positive, meaning she has a hepatitis B infection, then the infant should receive HBIG AND the hepatitis B vaccine within 12 hours of birth, regardless of birth weight.
- The vaccine and HBIG should be in separate limbs (one thigh for the HPV, the opposite thigh for HBIG) to maximize effectiveness.
- This combined approach dramatically lowers the risk that the baby becomes infected.
2. Mother whose HBsAg status is unknown at the time of delivery
If the mother’s infection status is unknown at the time of birth, then the risk is uncertain. The guidelines say:
- If the infant’s birthweight is ≥ 2,000 grams (≈4.4 lbs), then the baby gets the hepatitis B vaccine at birth (within 12 hours if possible), and the provider should try to get the mother’s HBsAg result as soon as possible.
If later the mother is found to be HBsAg-positive, then the baby must receive HBIG as soon as possible (and the vaccine dose stands).
- If the infant’s birthweight is < 2000 grams, then the uncertainty + low birthweight means the baby should receive both HBIG and the vaccine within 12 hours. This is because low birthweight babies respond less robustly to the vaccine alone and may be at higher risk.
3. Mother known to be HBsAg-negative
If the mother’s HBsAg test is clearly negative during this pregnancy, and the baby is of adequate weight, then the infant needs the hepatitis B vaccine at birth or by discharge, but HBIG is not required.
4. Very low birthweight (< 2000 grams) born to an HBsAg-negative mother
This is a special case. Some older guidelines said that for babies < 2000 grams born to HBsAg-negative mothers, the birth dose of vaccine might be delayed (at discharge or at age 1 month).
But for HBIG: if the mother is HBsAg-negative, HBIG is not indicated. The birth dose of the vaccine may be delayed if the weight is very low.
Why Does the Baby’s Birthweight Matter?
Birthweight (and gestational age) matter because:
- Low-birthweight or preterm infants have less mature immune systems and may respond less reliably to vaccines.
- In scenarios where the mother’s HBV status is unknown (or positive) and the infant is low birthweight, the guidelines recommend both vaccine + HBIG to increase protection.
- For low-birthweight babies born to HBsAg-positive mothers, the vaccine schedule may include 4 doses rather than 3. (starts at birth and requires an extra dose due to a lower response).
So birthweight is a key factor in decisions about HBIG.
Why Not Give HBIG to Every Single Baby?
You might wonder: Why not give HBIG to every newborn? Guidelines focus HBIG on infants at higher risk. Here are the reasons:
- The hepatitis B vaccine alone, when given at birth to infants of HBsAg-negative mothers, provides very strong protection. A universal birth-dose vaccine helps prevent horizontal (person-to-person) spread in early life as well.
- HBIG is a resource (cost, availability) and is only needed when there is a significant risk of infection (maternal HBV, unknown status with high risk, low birthweight).
- Unnecessary injections may cause avoidable discomfort, and they want to balance risk vs benefit.
- Evidence shows that in infants born to HBsAg-positive mothers, vaccine plus HBIG is superior to vaccine alone (94% vs ~75% effectiveness).
What Happens if HBIG Isn’t Given When Indicated?
If a baby who should have received HBIG (but didn’t) is exposed to HBV via a mother with infection, the risk is significant:
- Infants who become infected at birth are much more likely to develop chronic HBV infection (meaning lifelong) compared to children or adults who get infected later.
- Chronic infection leads to serious outcomes: liver cirrhosis, liver cancer, and early death.
- Delay in giving HBIG reduces its effectiveness—giving HBIG beyond 48 hours is much less protective.
Therefore, timely administration of HBIG (alongside vaccine) in at-risk infants is a credible preventive measure.
 What Exactly Is “Timely” for HBIG and HBV?
What Exactly Is “Timely” for HBIG and HBV?
When we talk about giving HBIG at birth, timing is key:
- For infants born to HBsAg-positive mothers, HBIG and the first dose of the hepatitis B vaccine should be given within 12 hours of birth, ideally.
- The vaccine dose is given in a separate limb from the HBIG. (HB vaccine in one thigh, HBIG in the other) to avoid interference.
- For unknown maternal status, if HBIG is needed (low birthweight), it should also be given within 12 hours.
- Giving HBIG and/or HP vaccine later (many hours delayed) reduces effectiveness.
Hence, every hospital and delivery team should have protocols to confirm maternal HBV status and administer the vaccine within this short time window.
Additional Important Details Parents Should Know
Vaccine Schedule After Birth Dose
Infants given the birth dose of hepatitis B vaccine and HBIG (when indicated) still must complete the full vaccine series. For infants born to HBsAg-positive mothers, after the birth dose, additional doses occur at 1 month, 2 months, 4 months, etc, depending on birthweight and vaccine type.
Same-day and next-day appointments available.
Post-vaccination serologic testing (PVST) is also recommended at age 9-12 months (or 1-2 months after the final dose if delayed) to check if the baby is protected (has anti-HBs) and not infected (HBsAg) if maternal infection existed.
Why Test at 9-12 Months?
Testing too early can detect passively transferred antibodies from HBIG or the mother and may give misleading results. So waiting until 9 months or later ensures accurate results.
What About Breastfeeding?
If a mother has an HBV infection (HBsAg positive) and everything has been done (infant gets HBIG + birth-dose vaccine, completes the series, and gets a follow-up test), breastfeeding is not contraindicated. It’s safe. The virus is not transmitted via breast milk in this context when prophylaxis is provided.
Communication and Documentation
Hospitals should have systems in place so that maternal HBV status (HBsAg) is known before or at delivery, the results are documented, and the newborn care team is alerted if prophylaxis (HBIG + HB vaccine) is needed.
As a parent, you may ask, “Has my baby’s first hepatitis B vaccine dose been given? Has HBIG been given (if needed)? Was it within 12 hours? Are we following the schedule?” It’s okay to ask these questions.
Special Scenarios: Home Births, Late Maternal Status, or “Unknown” Status
There are some real-world situations to consider. As a parent, ensure your baby’s pediatric provider knows these details and tracks follow-up.
😀 If the mother’s HBsAg status is only obtained after birth or results are delayed, the infant has already received the vaccine birth dose (but no HBIG), and normal birthweight, the infant may be given HBIG later (ideally as soon as the positive result is known). Protocols vary by region. The key is prompt action.
😀 If the baby is transferred (neonatal transfer) or the vaccination is delayed, extra doses and follow-ups may be needed.
😀 Low-birthweight infants are more complicated: if maternal status is unknown or positive, they should get HBIG and the HB vaccine within 12 hours. If maternal status is negative, then vaccine timing may be delayed until discharge or 1 month of age.
Step-by-Step: What You, as a Parent or Caregiver, Can Do
- Ask About Maternal HBV Testing: During pregnancy, ask your obstetric provider, “Have I been tested for hepatitis B (HBsAg) this pregnancy?” If yes, what were the results? This helps prepare the newborn team at delivery.
- Ensure Documentation at Delivery: When you arrive at the birthing facility, ensure your record includes the HBsAg result. If the result is pending or unknown, the clinical team should treat the baby as “unknown status” risk.
- At Birth, Ask About Prophylaxis: If the mother is HBsAg positive, ask, “Was HBIG given to the baby and the HB birth dose within the first 12 hours?” If the mother’s status was unknown or late results, and the baby is low birthweight, ask the same question.
- Track Vaccine Schedule: After the birth dose, make sure your baby completes the hepatitis B vaccine series. Confirm with your pediatric provider.
- Confirm Follow-Up Testing if Needed: If your baby was in the high-risk category (maternal HBsAg positive), the doctor should order post-vaccination serologic testing (HBsAg + anti-HBs) at age 9-12 months. Ask when this will happen.
- Keep the Vaccine Record and Baby’s Health Provider Informed: Keep copies of the birth dose information (date, vaccine lot, HBIG if given, and what injection site) and bring it to your baby’s well-visits.
- Ask About Long-Term Protection: If everything was done correctly, your baby is very likely protected. Discuss with your provider about long-term protection, particularly if there were any delays or low birthweight issues.
Frequently Asked Questions (FAQs)
Q: If the baby’s mother is HBsAg negative, why give the HBV at birth at all?
Ans: Because the birth dose of the vaccine is a safety net. It protects the baby not only from possible maternal transmission but also from early horizontal exposure (household contacts, early life exposures).
Q: If the mother is HBsAg positive and we missed the 12-hour window, can we still give HBIG later?
Ans: While earlier is always better, if HBIG is delayed beyond 12 hours, discussions with infectious disease or pediatric specialists are needed. The protective effect declines with delay.
 Q: Is the baby safe if the mother’s HBV DNA (viral load) was very low?
Q: Is the baby safe if the mother’s HBV DNA (viral load) was very low?
Ans: Maternal viral load is a factor for treatment in pregnancy, but for the newborn’s immediate prophylaxis, the rule remains: if the mother is HBsAg-positive mother → HBIG + vaccine. Confirm with the obstetric and pediatric infectious disease teams.
Q: Does giving HBIG interfere with other vaccines?
Ans: No. HBIG (and the HB vaccine) given at birth does not interfere with the timing of standard infant immunizations.
Q: What if we are in a country outside the US with different guidelines?
Ans: Country-specific guidelines may vary, but the principle is similar: if the mother has HBV infection or risk of infection, the baby needs immediate prophylaxis. Make sure to consult your local pediatrician/health authority and adapt the approach accordingly.
Why This Matters—The Big Emotional and Health Impact
Let’s connect the clinical details to real-life meaning:
- The birth of a baby is a joyful and emotional moment. But for a baby born to a mother with HBV, there’s a silent risk: without proper prophylaxis, the baby could acquire HBV and live with chronic infection for decades. That’s heavy for a parent.
- But there’s powerful good news: with the right steps (birth dose vaccine + HBIG when needed + complete series + follow-up), the baby’s risk of chronic infection is dramatically reduced. This means a healthier life ahead, less worry, fewer doctor visits, and less chance of liver disease later.
- By understanding which infants still need HBIG at birth, you, as a parent, become empowered. You can ask the right questions, advocate for your baby, and feel more confident during those first critical hours after birth.
- In a world filled with many decisions and hand-offs (labor and delivery team, nursery, pediatrician), being informed gives you a strong seat at the table.
Key Takeaways for Parents
😀 If the baby’s mother has confirmed hepatitis B infection (HBsAg positive), or the baby has low birthweight and maternal infection status is unknown, then the baby still needs HBIG + the hepatitis B vaccine right at birth.
😀 If the mother is HBsAg-negative, then your baby still gets the birth dose of vaccine—but not HBIG.
😀 Ask the right questions at birth, track vaccine doses and follow-up testing, and your baby’s protection will be strong.
😀 You are a key member of your baby’s health team. Being informed helps your baby start life off in the safest possible way.
Feel free to bookmark this guide, bring it to your pediatric appointments, and share it with your support network.


 1. Mother known to be HBsAg-positive
1. Mother known to be HBsAg-positive
 What Exactly Is “Timely” for HBIG and HBV?
What Exactly Is “Timely” for HBIG and HBV? Q: Is the baby safe if the mother’s HBV DNA (viral load) was very low?
Q: Is the baby safe if the mother’s HBV DNA (viral load) was very low?