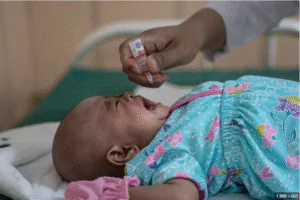
For many parents, hepatitis B feels abstract—just another scary disease on a long vaccine list. When parents hear the words “Hepatitis B” linked to their child, fear and confusion often follow. What is it? How serious can it be? And what really happens inside a child’s body when they face this infection?
fear and confusion often follow. What is it? How serious can it be? And what really happens inside a child’s body when they face this infection?
Hepatitis B is not just a medical term. It is a real fight happening deep inside the body—a battle between the virus and the child’s immune system. However, to make the best choices for your child, it is helpful to understand what actually happens when this virus enters a child’s body.
Here’s a parent-friendly walkthrough of how hepatitis B behaves—from the moment the virus enters the body to the possible outcomes, why it’s so dangerous, and why the vaccine is a critical line of defense. We’ll also explain prevention, treatment, and how families can step in to support a child fighting this infection.
What Is Hepatitis B and Why Should Parents Care?
Hepatitis B is a viral infection that targets the liver. The liver is one of the body’s most important organs. It helps filter toxins, stores energy, and regulates digestion. When hepatitis B attacks, it causes inflammation (swelling and irritation) in the liver. In children, this infection is especially concerning because:
- Their immune systems are still developing.
- They are more likely than adults to become chronic carriers of the virus.
- Long-term infection can lead to serious liver problems, like scarring (cirrhosis) or even liver cancer later in life.
Parents should know that Hepatitis B is preventable with a safe and effective vaccine. Yet, children who don’t get vaccinated or who are exposed at birth remain at risk.
The Hidden Journey—How Hepatitis B Infects a Child
The virus usually spreads in children through:
- Mother-to-child transmission during childbirth
- Exposure to infected blood or body fluids
- Unprotected household exposure, like sharing toothbrushes or open wound contact
Once inside, the virus starts its journey. Here’s what happens:
 Step 1—The Virus Enters
Step 1—The Virus Enters
Hepatitis B spreads through blood and certain body fluids. For babies and children, this can happen during birth, through daycare bites, playground scrapes, or even sharing grooming tools like nail clippers or toothbrushes. Once inside, the virus travels through the bloodstream and heads straight for the liver.
Step 2—Silent Invasion of the Liver
The virus attaches to liver cells (hepatocytes) and slips inside. There, it starts making copies of itself—hundreds of millions. At this stage, kids may look perfectly healthy. That’s the danger: the virus works silently. This “silent” stage is why parents may not know their child is infected.
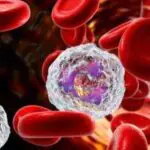
Step 3—The Immune System Reacts
After the virus settles in the liver, the child’s immune system recognizes the intruder. Here’s the tragic twist: White blood cells (immune system) rush in, releasing chemical signals to clear the virus. Instead, it causes inflammation, which damages the liver. This immune attack is a double-edged sword:
- It’s necessary to fight the virus.
- But it also causes the symptoms of Hepatitis B.
Some children may show warning signs such as:
- Fatigue (feeling very tired)
- Fever
- Nausea or vomiting
- Belly pain (especially on the right side, near the liver)
- Yellowing of the skin and eyes (jaundice)
- Dark urine or pale stools
Not every child will show these signs. In fact, most children remain symptom-free, making testing and screening very important.
The Possible Outcomes of Hepatitis B in Children
The body’s response to hepatitis B can lead to very different paths:
Step 4—Acute Infection—The Quick Fight
Some children fight off the virus within a few months. Their immune systems succeed, and the infection disappears. These children will then have lifelong immunity—their bodies will remember how to fight the virus if it ever returns.
Step 5—Chronic Infection – The Lingering Battle
For many children (up to 90%), especially babies infected at birth, the virus does not go away. The immune system fails to clear HBV. Instead, it becomes a chronic infection. The virus stays forever, quietly destroying the liver year after year, even decades.
Children rarely exhibit symptoms at this stage, though damage is already underway. These complications may not appear until adolescence or adulthood, but the foundation is laid in childhood infection. Over time, this silent infection may lead to:
- Cirrhosis: Permanent scarring that blocks liver function.
- Liver cancer: Hepatocellular carcinoma, one of the deadliest cancers worldwide.
- Liver failure: The liver stops working, often requiring a transplant.
This is why early detection, treatment, and prevention with vaccines are so critical.
Real-Life Analogy: Burglars and Cement
Think of HBV as burglars breaking into your home (the liver). At first, they’re quiet—you don’t even notice. Then your security system (the immune system) reacts, but instead of catching the burglars, it destroys the furniture and walls.
Over time, the damage becomes permanent—like pouring cement into the house (cirrhosis). That’s why prevention is so important. You don’t want the burglars getting in at all.
What Parents Can Expect During Diagnosis
Doctors can tell whether a child has an acute or chronic infection through these tests. Parents often find comfort in having clear answers, even if the diagnosis is scary. If a doctor suspects Hepatitis B, they may order:
- Blood tests to detect the virus and check liver function
- Ultrasounds to look for liver damage
- In rare cases, a liver biopsy (a small sample of liver tissue for closer study)
Treatment Options for Children with Hepatitis B
Currently, there is no single medicine that can completely “erase” Hepatitis B from the body. But doctors have strong tools that can help children live healthy lives while controlling the infection.
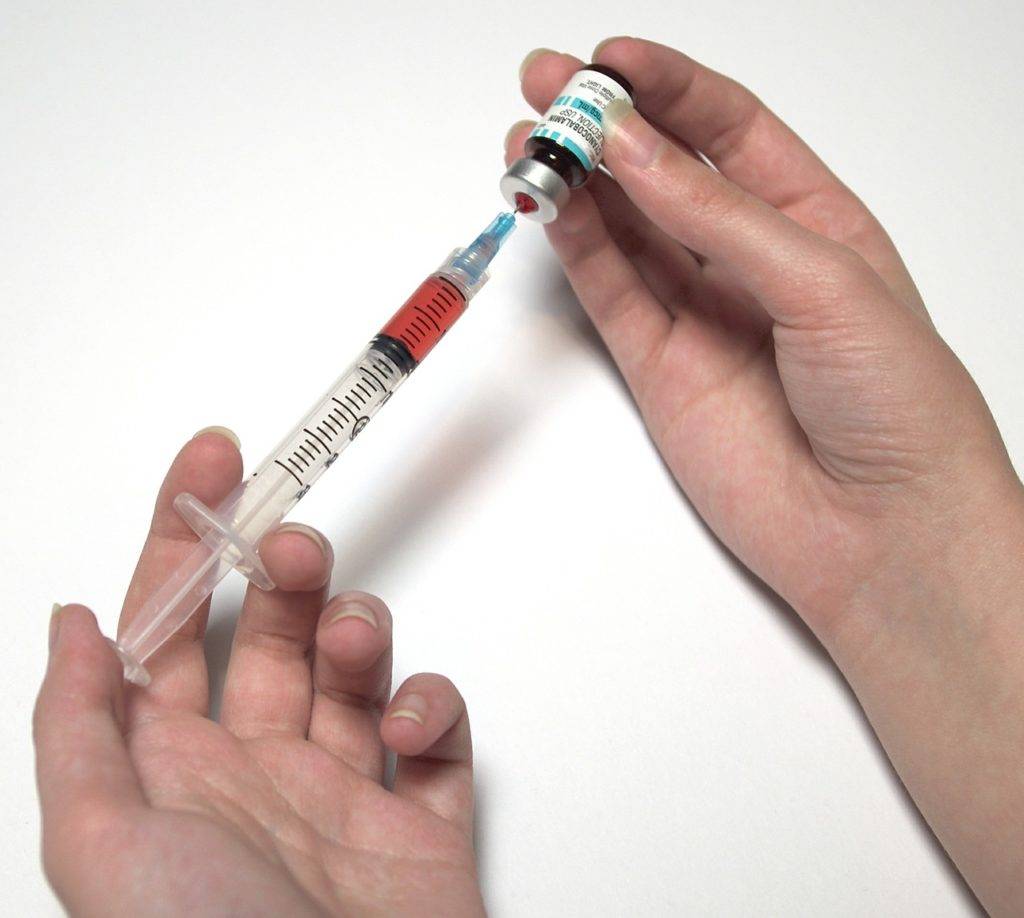
 Antiviral Medications
Antiviral Medications
Doctors may prescribe antiviral medicines that slow down the virus. These medications don’t cure Hepatitis B, but they reduce the amount of virus in the blood. This lowers the risk of liver damage and helps children stay healthier longer. Some antivirals are in pill form, while others may be given as injections.
Same-day and next-day appointments available.
Regular Monitoring and Check-Ups
Even if a child feels fine, Hepatitis B can still cause silent damage over time. That’s why doctors schedule regular blood tests and liver ultrasounds. These check-ups help catch problems early—before they turn into something serious.
Supportive Care at Home
Parents can make a big difference by creating a liver-friendly lifestyle for their child. This means:
- Serving a balanced diet full of fruits, vegetables, whole grains, and lean proteins.
- Encouraging daily physical activity to keep the immune system strong.
- Avoiding exposure to toxins, including alcohol and certain over-the-counter medications, can stress the liver.
With the right care plan, children with Hepatitis B can grow, thrive, and reach their full potential.
Prevention Is the Greatest Defense
The most powerful tool against hepatitis B isn’t medicine—it’s prevention. The vaccine is a simple shot that gives children protection for life.
- The Power of the Birth Dose: Experts recommend that every newborn receive the first dose of the hepatitis B vaccine within 24 hours of birth. This step alone prevents cases of mother-to-child transmission.
- Completing the Vaccine Series: The vaccine works best when given in a series of 3-4 doses. Parents should follow their child’s immunization schedule carefully, making sure no doses are missed.
- Protecting the Family Too: If one child in the home has Hepatitis B, other family members should also be tested and vaccinated if needed. This creates a circle of protection around the child and stops the virus from spreading further.
- Global Impact of Vaccination: Thanks to widespread vaccination programs, rates of childhood Hepatitis B infection are dropping worldwide. What was once a major cause of liver disease in children is now becoming rare in vaccinated populations.
Prevention through vaccines is one of the greatest public health victories of our time—and it’s a gift every parent can give their child.
Living with a Child Who Has Hepatitis B—Family Guidance
Caring for a child with Hepatitis B goes beyond doctor visits. It’s about creating a safe, loving, and supportive environment where your child can grow and thrive.
Reducing Transmission Risks at Home
Parents don’t need to isolate their child or treat them differently. Simple daily precautions can keep everyone safe. These small steps reduce the chance of spreading the virus while still allowing the child to live a normal life.
- Never share toothbrushes, razors, or nail clippers.
- Cover open cuts with bandages until they heal.
- Encourage regular handwashing with soap and water.
- Teach children not to share items that might carry blood or saliva.
Supporting Your Child at School
Children with hepatitis B can go to school just like everyone else. The virus is not spread through casual contact, such as hugging, playing, or sharing classroom space. Parents should:
- Inform the school nurse or health staff, especially if the child takes medication or needs regular check-ups.
- Advocate for their child’s privacy—schools should not single them out or treat them differently.
- Reassure teachers and caregivers that the child poses no risk through normal activities.
Building Friendships and Self-Confidence
Children with Hepatitis B sometimes feel “different” or even ashamed. Parents can help by:
- Encouraging open conversations about the illness in age-appropriate ways.
- Reminding children that they are healthy, capable, and loved.
- Supporting participation in sports, hobbies, and social activities that build self-esteem.
Planning for the Future
As children with Hepatitis B grow into teens and young adults, they’ll need to understand how to manage their health independently. Parents can prepare them by:
- Teaching the importance of regular doctor visits.
- Explaining why certain habits—like avoiding alcohol—protect their liver.
- Encouraging responsibility in informing future partners and taking precautions.
Offering Emotional Strength
Above all, children need to feel supported and understood. Parents should remind them:
- “This illness does not define who you are.”
- “With care and responsibility, you can live a full, happy life.”
- “We are in this together as a family.”
Hepatitis B is a part of their story, but it does not have to limit their future.
The Hope for the Future
The story of Hepatitis B is not one of despair—it’s one of progress and promise. Over the past few decades, the introduction of the Hepatitis B vaccine has already saved millions of lives worldwide.
Today, scientists are working tirelessly on new treatments and potential cures that could change the lives of children living with the infection. These breakthroughs are still being studied, but the progress is real. Some of the most exciting areas of research include
- Next-generation antivirals that target the virus more effectively with fewer side effects.
- Immune-boosting therapies are designed to help the body recognize and naturally destroy the virus.
- Gene-editing research (like CRISPR) could one day completely remove the virus from infected cells.
Each year, doctors and researchers gain new tools to help children live longer, healthier lives with hepatitis B. For parents, this means that while the diagnosis may feel overwhelming today, the future holds real hope.
Families can take comfort in knowing that medicine is advancing, and children with Hepatitis B can look forward to brighter, healthier tomorrows.
FAQ—What Happens in Hepatitis B Infection
Q1: Can children with hepatitis B look healthy for years?
Yes. Many infected children show no outward symptoms while their liver is being damaged.
Q2: Why do babies get chronic hepatitis B more often than adults?
A baby’s immune system is immature and often can’t clear the virus, leading to lifelong infection.
Q3: What’s the difference between acute and chronic infection?
“Acute” means a short-term infection that may clear. Chronic means the virus stays in the body for life.
Q4: What are the long-term risks of chronic hepatitis B?
Cirrhosis, liver cancer, and liver failure—sometimes appearing decades later.
Q5: Can medicine cure hepatitis B once a child is infected?
No. Treatments can manage it, but there is no cure. Vaccination is the only sure protection.
Inside the Battle, There is Always Hope
Hepatitis B isn’t just another line on a vaccine chart. It’s a virus that silently wrecks the liver, sets the stage for cancer, and shortens lives. But with a simple vaccine at birth and completed on schedule, you can stop the invasion before it begins. When a child faces hepatitis B, it may feel like an invisible war inside their body.
But parents are not powerless. With early detection, medical care, healthy living, and vaccines, families can fight back. The most important weapon? Knowledge. By understanding what happens inside the body during Hepatitis B, parents can protect their children today and help ensure a healthier future.
Key Takeaways for Parents
- Hepatitis B is a viral infection that attacks the liver.
- Many children do not show symptoms, making screening essential.
- Some children recover completely, but many—especially infants—develop chronic infection.
- Long-term Hepatitis B can cause liver damage and cancer if untreated.
- The Hepatitis B vaccine is safe, effective, and lifesaving.

 Step 1—The Virus Enters
Step 1—The Virus Enters
 Antiviral Medications
Antiviral Medications